Nursing alumnae help save New York

May 4, 2020 – While many Texans have not seen the effects of COVID-19 up close, Courtney Waddle (BS ’12) and Maybelle Anderson (BS ’12) signed up for it. The registered nurses joined three other colleagues to travel to the epicenter of COVID-19 in the United States: New York City, where infections number more than 10 times that of the entire state of Texas.
After they landed in New York on April 3, Anderson stayed until Tuesday, April 28 while Waddle plans to stay through May 9. Throughout their stay, it has been hard for them to sleep as they wondered whether patients they cared for one day would be there the next. There was concern for safety because the personal protective equipment shortage was so bad that some nurses hoarded it. Then there was death.
Why go?

“They needed our help,” Waddle said. “I felt worthless sitting around. I have all these skills and I wanted to use them to help.”
Both Waddle and Anderson were furloughed by Lonestar Endoscopy in Flower Mound and Southlake. Lonestar had to shut its doors because most of the center’s surgeries were considered elective. That was the first in a string of events that propelled Anderson to go.
“For every reason I said no, it changed,” said Anderson. “It’s a God thing. I definitely would have just stayed home, but everything I needed kept coming in.”
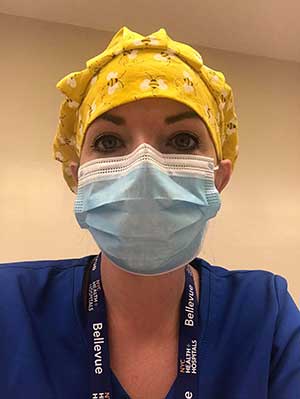
Anderson wears a specific protective face mask, a 3M 1870, as opposed to the traditional N95 mask due to the fit of her face. She was concerned about supply but a friend gave her five of them.
“It’s a sign, I thought. Just go,” she said.
Face shields were delivered to the group, which can be followed on Facebook at TX RNs Take on NY, right before their flight.
Anderson was surprised not just at herself, but other nurses.
“We don’t know why we’re here, but we’re here. We keep waking up to do it the next day,” Anderson said. “It’s an unreal experience for all of us.”
When they landed in the city, it was mostly empty except for Central Park. No social distancing. No masks.
Anderson asked her friends, “Don’t they realize their city is dying?”
The work

Both nurses worked 12-hour shifts. Waddle works at Bellevue Hospital in Manhattan, the oldest public hospital in the U.S. while Anderson was on the night shift at Coney Island Hospital in Brooklyn with a few nights spent working in a tent set up outside for overflow. Despite feeling prepared for what they were stepping into, they were still surprised at the fallout from COVID-19.
“It’s unlike anything else,” said Anderson.
Waddle added: “It’s shocking when someone is just not there the next day. It’s hard to sleep because I have a lot of fear and worry about whether patients will be there when I go back to work.”
Patients stacked up in the intensive care unit. In the same half hour, two of Waddle’s patients required rapid response and were moved to the ICU. When she took the second one, she was surprised to see a third patient already in the ICU who had been doing well the previous day.
Anderson described an even more rapid decline. She saw a 45-year-old talking on the phone normally with his family. Within 20 minutes, he died from a blood clot common in COVID-19 patients.
“I don’t think people can relate to what I’m saying. This is something you never want to see,” Anderson said. “It doesn’t discriminate. Without eyes on it, you can’t fathom how bad it is.”
“It’s scary. People at home just seem annoyed by the whole thing,” Waddle said. “I know it’s mostly an inconvenience for them, but people are dying in New York. Right now, the inconvenience is worth it.”
There were many challenges. Coney Island Hospital opened a ward that hadn’t been used in 15 years. The supply shortage forced nurses to grab masks and personal protective equipment (PPE) whenever they could. The nurse-to-patient ratio reached 1-to-25 and higher, providing no time to comfort patients.
“We’re constantly moving,” said Waddle.
Amid the chaos, both Waddle and Anderson found themselves recalling lessons learned at Texas Woman’s University. Every time she put in an IV line, Waddle thought back to the specific way Professor Nola Schrum showed her to prime the line.
Anderson remembered one of her most embarrassing mistakes she made as a nursing student while changing a catheter bag, leaving the floor covered in urine.
“You know what they say: once you learn from a mistake, you’ll never make it again. That’s the truth!” she said with a chuckle.
Anderson plans to return to TWU this fall to become a family nurse practitioner.
Positive moments

Each nurse found reasons to stay positive. Waddle was able to discharge her first patient on April 15, the first full recovery she had seen.
“It was a good day.”
Meanwhile, Anderson built a relationship with a patient she visited on her break every morning around 4 a.m. At first, the patient wasn’t expected to recover. She fit the profile of those most susceptible to COVID-19.
“But she gets better and better every day,” said Anderson.
On their visits, they ended up laughing. The last time they did, Anderson was worried the noise would wake other patients in the early hour.
“She told me not to worry. She said that I was the only voice they’d heard in days. They needed to hear the laughter,” said Anderson.
Patients weren’t allowed visitors because of how easily the virus is transmitted. Most medical professionals patients see were almost fully covered in PPE. There was no opportunity for personal connection.
“I try to give as much as I can to these patients. An extra five minutes here and there just to talk with them, stand with them. It makes them so thankful,” Waddle said. “A little can mean a lot.”
Sometimes the extra effort came with no words, just a look.
“I’ve never looked into a patient’s eyes like I do here. There is real fear down to their soul. Everyone who comes in with COVID-19 is afraid they are going to die,” Anderson said. “I’ll never forget their eyes. It’s a rare thing to be able to look at someone, read the fear in their eyes and let them know I understand and am there to help them.”
Staying sane
New York nurses belong to a union that provides benefits Texas nurses didn’t anticipate. They received a full hour for lunch, sometimes an hour and a half according to Anderson.
Working in Manhattan, Waddle takes the opportunity to walk the city and clear her mind. It’s easier to do with the streets so empty.
Anderson typed out a journal about the day on her computer. Then she deleted it.
“It’s therapeutic. It’s the only real outlet I have outside of talking with the five of us from Texas.”
Both of them enjoyed rides to and from work on the bus, occasionally escorted by New York police. Nurses from across the country and abroad let loose on the bus after shifts. They made jokes they had been holding in all day. They shared stories. They laughed. They built friendships.
“Meeting people I work with has been a really positive experience. None of us have to risk our lives to be here, but my group is amazing,” Anderson said of the 25 nurses on her shift. “Even our bus driver.”
Her bus driver was a volunteer pastor from Kansas.
What now?
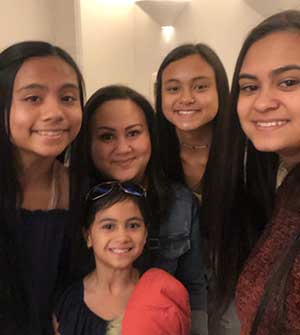
Waddle and Anderson both expressed concern that others misunderstand the significance of the fight against COVID-19. Waddle feared that people she knows in Texas weren’t taking the pandemic seriously enough. When she returns, she’ll quarantine herself on the second floor of her house.
“It’s crazy that they’re opening everything up. There isn’t a cure yet,” said Anderson. “I honestly think going back to normal will unleash a new cycle. There’s no doubt in my mind that it’s going to happen.”
Their original commitment ended Saturday, April 25. Anderson stayed through the following Tuesday, April 28 while Waddle is there until Saturday, May 9.
Both have families that have waited on them to return. Waddle’s husband is a firefighter who picked up extra shifts to fill the void. Anderson’s four daughters were staying with their father.
Anderson’s youngest, an 8-year-old, asked every now and then, “How many sleeps until you come home?” Now Anderson waits until her two-week quarantine ends to tuck her in at night.
Media Contact
Joshua Flanagan
Digital Content Manager
940-898-3436
jflanagan1@twu.edu
Page last updated 3:46 PM, September 27, 2021